 Manual therapists usually have a toolbox of various techniques at their disposal to help release and relax muscles, which will then assist the client's body to promote the healing mechanisms.
Manual therapists usually have a toolbox of various techniques at their disposal to help release and relax muscles, which will then assist the client's body to promote the healing mechanisms.
METs are unique in their application in that the client provides the initial effort and the practitioner just facilitates the process. The primary force comes from the contraction of the client's soft tissues (muscles), which is then utilized to assist and correct the presenting musculoskeletal dysfunction.
This treatment method is generally classified as a direct form of technique as opposed to indirect, since the use of muscular effort is from a controlled position, in a specific direction, and against a distant counterforce that is usually offered by the therapist.
🔹BENEFITS OF MET
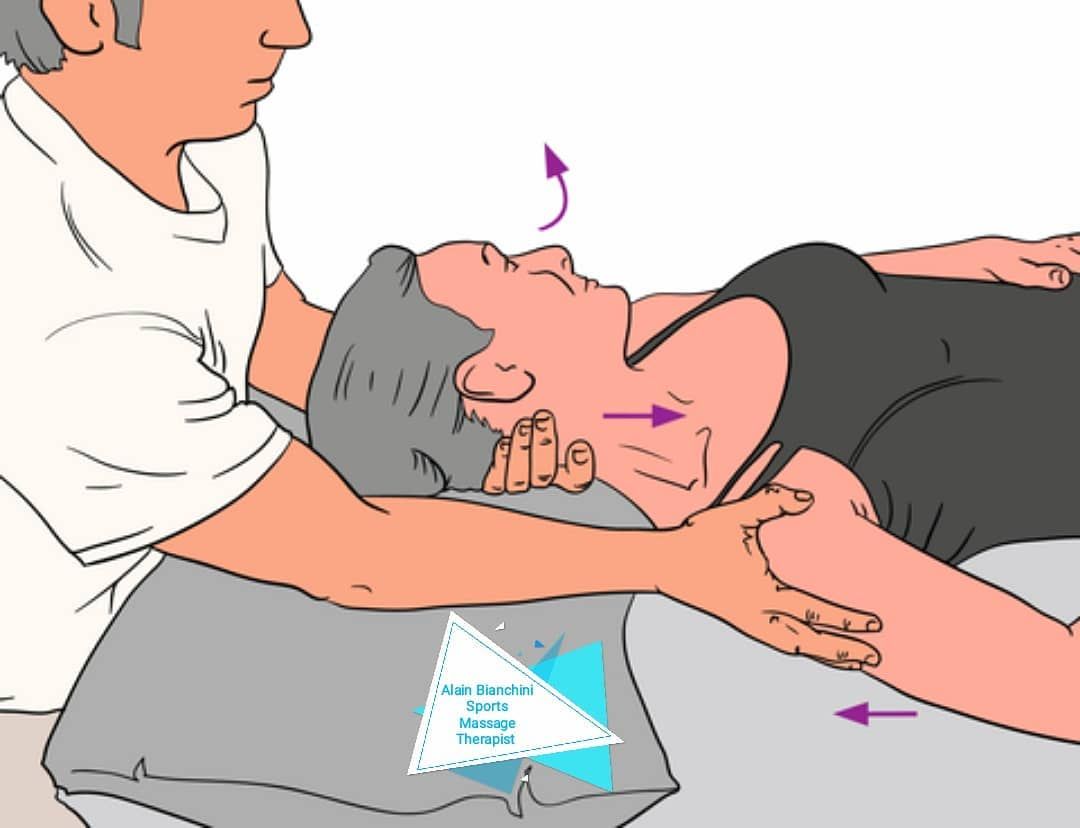
Acording to John Gobbons one of the benefits of METs is their use in normalizing joint range, rather than in improving flexibility. This might sound counterintuitive. However what he is saying is if, for example, your client cannot rotate their neck (cervical spine) to the right as far as they can to the left, they have a restriction of the cervical spine in a right rotation.
The normal rotational range of the cervical spine is 80 degrees, but let’s say the client can only rotate 70 degrees to the right. This is where METs come in.
After an MET has been employed on the tight restrictive muscles, hopefully the cervical spine will then be capable of rotating to 80 degrees - the patient has made all the effort and you, the practitioner, have encouraged the cervical spine into further right rotation. You have now improved the joint range to “normal.”
This is not stretching in the strictest sense - even though the overall flexibility has been improved, it is only to the point of achieving what is considered to be a normal joint range.
Depending on the context and the type of MET employed, the objectives of this treatment can include:
🔸Restoring normal tone in hypertonic muscles 🔸Strengthening
Whiplash is a common injury that occurs within the neck from a sudden acceleration and deceleration force causing unrestrained, rapid movements backward and forward to the head and the neck, which is often from a car accident. Whiplash injuries are those that damage the soft tissues and the bone structures, while a whiplash associated disorder describes a more chronic and severe condition. Thankfully, whiplash isn’t a life-threatening injury, but it can wind up leading to a prolonged period of disability. Even though the majority of individuals who are in a minor car accident will recover quickly without worrying about any chronic symptoms, there are some who will continue experiencing symptoms for years after the accident occurred. Whiplash is commonly caused by a car accident where the individual is in a car that isn’t moving and they are struck by another car from behind. The rear impact causes the neck and head to be forced into a hyperextended position as the seat pushes the individual forward and the head and neck end up falling backward. After a small amount of time, the neck and head will recover and be thrown into a forward position.
Whiplash is commonly known as whiplash associated disorder because often it is not just the neck affected, but other areas. Most commonly the shoulder and back are affected with a whiplash. A common shoulder problem is known as shoulder impingement syndrome and it is unclear why this can occur following road traffic incidents, but doctors are aware that it can cause difficulty sleeping on the affected side, difficulty lifting your arm above your head, and reaching behind your back.
Whiplash and Whiplash Associated Disorder (WAD) Anatomy Inside of the spinal column, there is a tube for the spinal cord. This thick bundle of nerves starts at the base of the brain. It relays information between the brain and the body. Nestled between the vertebrae are the discs. Each individual disc is attached to the bottom of the vertebra that lies above it and the top of the one below it. Muscles and strong ligaments keep the column together. All of the structures work together to surround, protect and support the spinal cord.
How to Treat Whiplash and Whiplash Associated Disorders:
Tips: • Don’t immobilize the injured site. This causes the muscles to stiffen and slow the healing process down. If you do need to wear a neck collar, use it only for short term (24-48 hours) and remove it when symptoms start to improve. Remember you need to regain mobility to the neck. • Get back to normal daily routine including your job as soon as you can. This has been shown to be beneficial in speeding up recovery.